
Integrated Health Care Report
: Analysis on the Market, Trends, and TechnologiesThe integrated patient-care market recorded $23,320,000,000 in 2024, and is projected to expand at a 14.2% CAGR to $45,400,000,000 by 2029, driven by rising adoption of value-based contracts, interoperability mandates, and expanded remote-care models. Market forecasts and vendor analyses indicate strong software-led growth (platforms and integration engines) while news and deal activity show payers and health systems consolidating to capture downstream value Healthcare Integration Market Report and Forecast 2025-2034.
The last update of this report was 7 days ago. If you spot incomplete or incorrect info, please let us know.
Topic Dominance Index of Integrated Health Care
The Topic Dominance Index analyzes the time series distribution of published articles, founded companies, and global search data to identify the trajectory of Integrated Health Care relative to all known Trends and Technologies.
Key Activities and Applications
- Value-Based Contract Enablement: Deploying data and care-coordination platforms to measure quality, close gaps, and trigger outcome-based payments; platforms often combine CCM, RPM, and coding/risk-adjustment workflows.
- Behavioral-Physical Health Synchronization: Embedding behavioral specialists and digital behavioral tools into primary care workflows to manage comorbidity and reduce acute escalations.
- Home-First Chronic Care: Shifting longitudinal management into the home using RPM, virtual multidisciplinary visits, and home-care benefit management to lower utilization and manage risk
- Interoperability & Compliance Services: Delivering FHIR/HL7 implementation, data normalization, and ONC compliance modules as a commercial service to reduce provider integration burden
- Population Health & SDOH Orchestration: Aggregating clinical, claims, and SDOH inputs to stratify risk and prioritize outreach for high-cost cohorts, particularly within FQHCs and safety-net networks i2i Population Health.
Emergent Trends and Core Insights
- Platform consolidation by payers and systems is intensifying: payer-led acquisitions of primary-care assets and investments in navigation platforms aim to lock patient flows and capture margin, while specialized vendors sell essential integration components U.S. Integrated Delivery Network Market.
- AI is moving from administrative to prescriptive tasks: predictive risk engines and workflow automation are now being trialed to recommend care sequences and trigger social-care referrals within care plans.
- Safety-net and FQHC networks are experimentation hubs: these organizations demonstrate rapid SDOH integration and community routing that larger systems are starting to replicate for equity-focused contracts The Institute for Family Health.
- Tele-behavioral health scale is a tactical response to workforce shortages: growing telepsychiatry deployments bridge demand but emphasize measurement-based care and regulatory compliance for reimbursement.
- Payment-layer integration remains underdeveloped relative to clinical integration; real-time adjudication and incentive embedding represent an immediate value creation opportunity for middleware providers.
Technologies and Methodologies
- FHIR/HL7-First Integration Engines: plug-and-play adapters and normalization stacks that reduce project timelines and enable multi-vendor interoperability.
- AI-Driven Care Orchestration: models that ingest longitudinal EHR, claims, RPM, and SDOH to produce prioritized actions for care teams; used for risk stratification and appointment routing.
- Remote Patient Monitoring + Virtual Hub: end-to-end RPM platforms tied to virtual clinical workflows and escalation protocols that reduce readmissions and enable home-first pathways
- Outcome-Linked RCM and RPA: automation of claims adjudication and quality metric tracking to support value-based payments and reduce revenue leakage HealthCare Information Management, Inc. (HCIM).
- Integrated Patient Engagement Libraries: curated digital content and pathways (education, portals, triage) that lower demand and standardize self-management across conditions
Integrated Health Care Funding
A total of 621 Integrated Health Care companies have received funding.
Overall, Integrated Health Care companies have raised $58.8B.
Companies within the Integrated Health Care domain have secured capital from 1.8K funding rounds.
The chart shows the funding trendline of Integrated Health Care companies over the last 5 years
Integrated Health Care Companies
- CircleLink Health — CircleLink Health offers an AI-enabled care-management platform focused on enrollment, engagement, and gap-closure for Medicare programs; deployments report high patient satisfaction rates and measurable revenue capture from APCM/CCM programs. The company combines automated outreach with RN oversight to drive adherence and quality metrics, positioning itself as a plug-in partner for practices facing value-based contract stress
- Integrated Healthcare Ai Inc. — Integrated Healthcare Ai Inc. provides one-click FHIR services and ONC HTI-1 compliance tooling aimed at small/mid EHR vendors, converting regulatory friction into a commercial product. Their usage-based pricing lowers barrier to ONC certification and accelerates customers' time-to-market for interoperable features
- Integrated Home Care Services, Inc. — Integrated Home Care Services, Inc. (IHCS) is a benefits manager and home-care operator serving 2.7 million patients across 13 states, using a proprietary MedTrac platform to reduce avoidable hospitalizations and support payer contracting. Their position as an outcomes-oriented home platform makes them a likely target for payers seeking to shift utilization to lower-cost settings
- HCI — HCI operates a CONNECTPlus patient-education and engagement library with over 1,000 clinician-facing assets and pathway automation that demonstrably reduces referrals and waiting-list pressure for NHS clients. Their model shows how content + workflow can materially reduce demand while preserving clinical safety
- Healthcare Integrations, LLC — Healthcare Integrations, LLC specializes in Mirth, HL7, FHIR and lab/EHR connectors as consulting and managed services, positioning it as an acquisition target for larger systems that need integration teams and middleware expertise. Their low-cost, high-velocity integration work helps providers meet interoperability deadlines with less internal overhead
TrendFeedr’s Companies tool is an exhaustive resource for in-depth analysis of 4.1K Integrated Health Care companies.
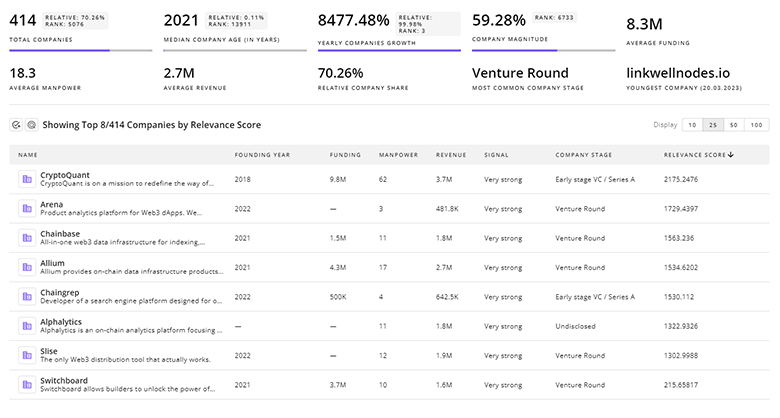
4.1K Integrated Health Care Companies
Discover Integrated Health Care Companies, their Funding, Manpower, Revenues, Stages, and much more
Integrated Health Care Investors
The TrendFeedr’s investors tool features data on 2.0K investors and funding activities within Integrated Health Care. This tool makes it easier to analyze complex investment patterns and assess market potential with thorough and up-to-date financial insights.
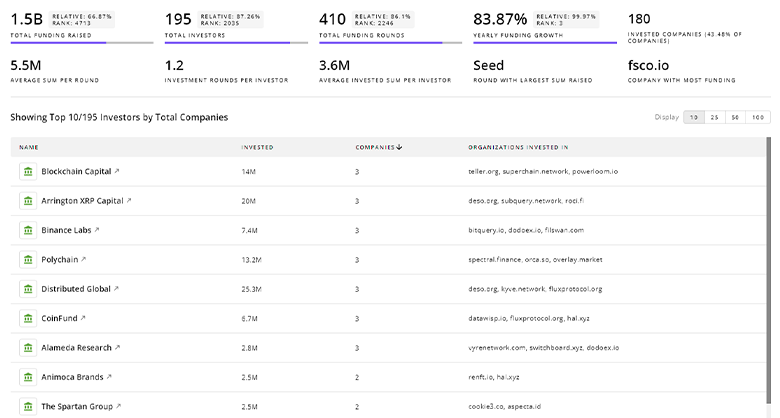
2.0K Integrated Health Care Investors
Discover Integrated Health Care Investors, Funding Rounds, Invested Amounts, and Funding Growth
Integrated Health Care News
Stay ahead of the curve with Trendfeedr’s News feature. The tool provides access to 959 Integrated Health Care. Navigate the current business landscape with historical and current Integrated Health Care data at your fingertips.
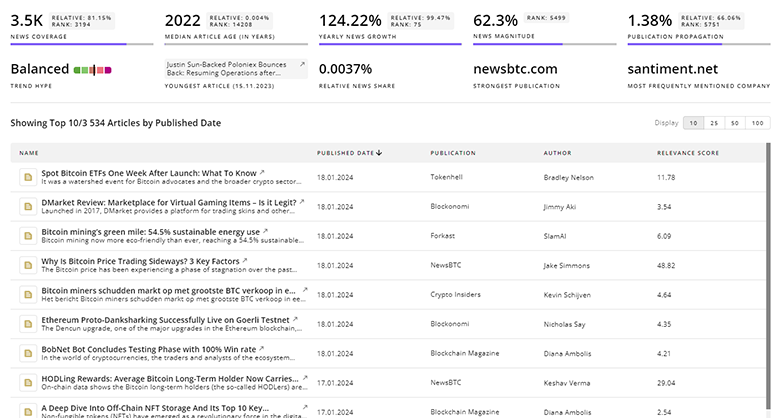
959 Integrated Health Care News Articles
Discover Latest Integrated Health Care Articles, News Magnitude, Publication Propagation, Yearly Growth, and Strongest Publications
Executive Summary
Integrated health care is now a competition for data-flow control and service orchestration, not merely a set of coordination projects. The market presents two clear commercial pathways: build end-to-end platform control (vertical consolidation by payers and large systems) or become an indispensable integration ingredient (specialist middleware, AI orchestration, home-care platforms). Financial upside concentrates around three capabilities: reliable interoperable data normalization, prescriptive analytics that drive measurable outcomes, and modular operational services (virtual CCM, RPM, behavioral staffing) that convert clinical performance into value-based revenue. Organizations that align incentives across clinical, social, and financial layers while securing certified integration capabilities will materially improve margins and patient outcomes in the next 18 months.
If you’re an expert in trends or emerging tech, we invite you to contribute to our insights.











